Do you need a Dermatology appointment?
The Most Common Skin Cancer – Basal Cell Carcinoma
 Basal cell carcinoma (BCC) is the most common form of skin cancer and the most frequently occurring form of all cancers. In the U.S. alone, more than 4 million cases are diagnosed each year. BCCs arise from abnormal, uncontrolled growth of basal cells.
Basal cell carcinoma (BCC) is the most common form of skin cancer and the most frequently occurring form of all cancers. In the U.S. alone, more than 4 million cases are diagnosed each year. BCCs arise from abnormal, uncontrolled growth of basal cells.
Because BCCs grow slowly, most are curable and cause minimal damage when caught and treated early. Understanding BCC causes, risk factors and warning signs can help you detect them early, when they are easiest to treat and cure.
What is a basal cell carcinoma?
One of three main types of cells in the top layer of the skin, basal cells shed as new ones form. BCC most often occurs when DNA damage from exposure to ultraviolet (UV) radiation from the sun or indoor tanning triggers changes in basal cells in the outermost layer of skin (epidermis), resulting in uncontrolled growth.
What does Basal Cell Carcinoma look like?
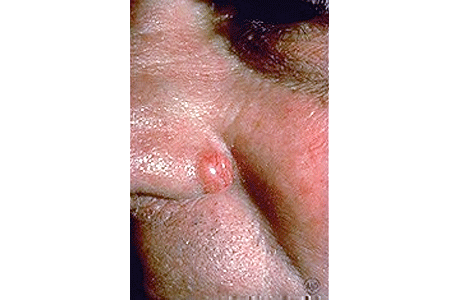
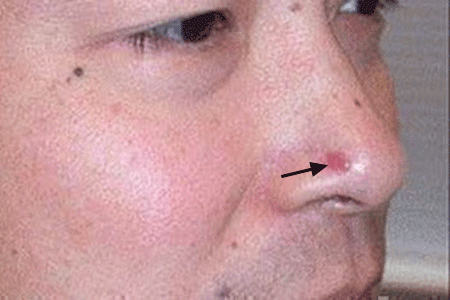 BCCs can look like open sores, red patches, pink growths, shiny bumps, scars or growths with slightly elevated, rolled edges and/or a central indentation. At times, BCCs may ooze, crust, itch or bleed. The lesions commonly arise in sun-exposed areas of the body. In patients with darker skin, about half of BCCs are pigmented (meaning brown in color).
BCCs can look like open sores, red patches, pink growths, shiny bumps, scars or growths with slightly elevated, rolled edges and/or a central indentation. At times, BCCs may ooze, crust, itch or bleed. The lesions commonly arise in sun-exposed areas of the body. In patients with darker skin, about half of BCCs are pigmented (meaning brown in color).
It’s important to note that BCCs can look quite different from one person to another.
How dangerous are Basal Cell Carcinomas (BCC)?
While BCCs rarely spread beyond the original tumor site, if allowed to grow, these lesions can be disfiguring and dangerous. Untreated BCCs can become locally invasive, grow wide and deep into the skin and destroy skin, tissue and bone. The longer you wait to have a BCC treated, the more likely it is to recur, sometimes repeatedly.
There are some highly unusual, aggressive cases when BCC spreads to other parts of the body. In even rarer instances, this type of BCC can become life-threatening.
How widespread is BCC?
Basal cell carcinoma is quite common, and the number of reported cases in the U.S. has steadily increased.
More than 4 million Americans are diagnosed with BCC each year.
More than one out of every three new cancers are skin cancers, and the vast majority are BCCs.
The diagnosis and treatment of non-melanoma skin cancers, including BCC and squamous cell carcinoma (SCC), increased up to 77 percent between 1994 and 2014.
Basal Cell Carcinoma Risk Factors
 Basal cell carcinoma (BCC) is caused by damage and subsequent DNA changes to the basal cells in the outermost layer of skin. Exposure to ultraviolet (UV) radiation from the sun and indoor tanning is the major cause of BCCs and most skin cancers.
Basal cell carcinoma (BCC) is caused by damage and subsequent DNA changes to the basal cells in the outermost layer of skin. Exposure to ultraviolet (UV) radiation from the sun and indoor tanning is the major cause of BCCs and most skin cancers.
Understanding what causes BCC and the factors that increase your risk of getting it can help you prevent the disease or detect it in its earliest stages, when it’s easiest to treat.
These factors increase your BCC risk:
- UV exposure from the sun or indoor tanning.
- History of skin cancer, including squamous cell carcinoma (SCC) or melanoma.
- Age over 50: Most BCCs appear in people over age 50.
- Fair skin: People with fair skin have an increased risk.
- Male gender: Men are more likely to develop BCC.
- Chronic infections and skin inflammation from burns, scars and other conditions.
What causes basal cell carcinoma?
- UV exposure
- Almost all BCCs occur on parts of the body excessively exposed to the sun. Occasional extended, intense sun exposure that leads to sunburn and cumulative sun exposure over your lifetime are the main causes of skin damage that can lead to BCCs.
- The more time you spend in the sun, from beach vacations to walking the dog, the greater your likelihood of developing BCC. If your occupation requires long hours outdoors or if you spend your leisure time in the sun, your risk increases even more.
- Fortunately, UV exposure is a controllable risk factor.
- Indoor tanning
- Tanning beds emit UV radiation that is dangerous and raises your risk of developing BCC.
- More than 419,000 cases of skin cancer in the U.S. each year are linked to indoor tanning, including about 245,000 BCCs.
- People who have ever tanned indoors have a 29 percent increased risk of developing BCC.
- Any history of indoor tanning increases your risk of developing BCC before age 40 by 69 percent.
- Skin cancer history
- If you’ve already had a BCC, you are at risk for developing others over the years, either in the same area or elsewhere on the body. You are also at increased risk of developing other forms of skin cancer, including squamous cell carcinoma (SCC)and melanoma.
- Age over 50
- As you age, you accumulate sun exposure and sun damage, raising your risk of developing BCC. In the past few decades, the number of new BCC cases has increased sharply and the average patient age has steadily decreased. Today, dermatologists report that more 20- and 30-year-olds are being treated for BCCs, a trend that experts attribute to increased outdoor UV exposure and indoor tanning.
- Fair skin
- All people with a history of sun exposure or indoor tanning can develop BCC. However, people with fair skin, blond or red hair, blue, green or grey eyes, or skin that freckles or easily burns are at highest risk.
- The threat of skin cancer still exists for people with darker skin tones, and their need for sun safety is also absolutely essential.
- Gender
- Men with BCC continue to outnumber women with the disease, but more women are now getting BCCs than in the past.
- Skin injuries, inflammation or infection
- On rare occasions, BCCs develop on areas unexposed to UV radiation. In very rare cases, exposure to other forms of radiation or certain chemicals, chronic inflammatory skin conditions and complications of burns, scars or infections can be contributing factors.
What you can do
 Check your skin monthly: Perform thorough self-exams and visit your dermatologist regularly for professional skin exams.
Check your skin monthly: Perform thorough self-exams and visit your dermatologist regularly for professional skin exams.
Protect against UV rays: You can reduce your risk of getting BCC and other forms of skin cancer by taking simple, smart protective measures.
Fortunately, UV exposure is a controllable risk factor.
BCCs can be tricky
Keep in mind that BCCs can also look different from the descriptions above. In some people, BCCs can resemble noncancerous skin conditions such as psoriasis or eczema. Other times, the condition is diagnosed when a cut from shaving does not heal. In patients with darker skin, about half of BCCs are pigmented (meaning brown in color).
When in doubt, check it out. Follow your instincts and visit your dermatologist if you see anything new, changing or unusual on your skin.
If you’ve already had a BCC, you have an increased chance of developing another, especially in the same sun-damaged area or nearby.
A BCC can recur even when it has been carefully removed the first time, because some cancer cells may remain undetectable after surgery and others can form roots that extend beyond what’s visible. BCCs on the nose, ears and lips are more likely to recur, usually within the first two years after surgery.
Here’s what you can do to detect a recurrence and safeguard yourself against further skin damage that can lead to cancer:
- Be on the lookout: Pay particular attention to any previously treated site, note changes and consult with your dermatologist. If the BCC does return, your doctor may recommend a different type of treatment, such as Mohs surgery, a highly effective way to prevent and treat recurrences.
- Check yourself head to toe: Look for new or changing lesions that grow, bleed or do not heal. Learn how to check your skin.
- See your dermatologist annually for a professional skin exam. Self-exams do not take the place of a specialist who is skilled at identifying and treating abnormal skin growths.
- Follow up: If you’ve already had either BCC or squamous cell carcinoma (SCC), or a pre-cancer like actinic keratosis, be sure to see your doctor at recommended intervals.
- Be sun-safe every day of the year:Avoid unprotected UV exposure, seek the shade, especially when the sun is strongest and use a broad-spectrum sunscreen, a wide-brimmed hat and UV-blocking sunglasses. Safeguarding yourself every day is the single most effective way to reduce your risk of developing skin cancer. Get more skin cancer prevention guidelines.
Treatment
When detected early, most basal cell carcinomas (BCCs) can be treated and cured. Prompt treatment is vital, because as the tumor grows, it becomes more dangerous and potentially disfiguring, requiring more extensive treatment. Certain rare, aggressive forms can be fatal if not treated promptly.
If you’ve been diagnosed with a small or early BCC, a number of effective treatments can usually be performed on an outpatient basis, using a local anesthetic with minimal pain. Afterwards, most wounds can heal naturally, leaving minimal scarring.
Treatment options include:
- Curettage and electrodesiccation (electrosurgery)
- Mohs surgery
- Excisional surgery
- Radiation therapy
- Photodynamic therapy
- Cryosurgery
- Topical medications
- Oral medications for advanced BCC
Please visit our Skin Cancer Treatment page for more detail on the above treatments.
