Ready to schedule a dermatology appointment?
Atopic Dermatitis
Atopic Dermatitis (AD) is very common in children and babies, but also shows in adults. Many people also call this skin condition Eczema.
Children often get AD during their first year of life. If a child gets AD during this time, it shows as dry and scaly patches appear on the skin. These patches often appear on the scalp, forehead, and face. These patches are very common on the cheeks.
No matter where it appears, AD is often very itchy. Infants may rub their skin against bedding or carpeting to relieve the itch. In children of all ages, the itch can be so intense that a child cannot sleep. Scratching can lead to a skin infection.
Because atopic dermatitis can be long lasting, it is important to learn how to take care of the skin. Treatment and good skin care can alleviate much of the discomfort.
Atopic dermatitis (AD) looks different in infants, children, and adults. The following gives you the signs (what you see) and symptoms (what you feel) for each age group.
What AD looks like in Infants
AD can begin early. A child may be 2 or 3 months old when AD begins. When AD begins early, it often causes:
- A rash that appears suddenly and:
- makes the skin dry, scaly, and itchy
- forms on the scalp and face, especially on the cheeks (can appear on other areas of the body)
- can bubble up, then ooze and weep fluid
- causes itching that may come and go
- Rubbing against bedding, carpeting, and other things in order to scratch the itch
- Trouble sleeping
- Skin infections, common due to rubbing and scratching
Parents often worry that their babies are getting AD in the diaper area. A babies rarely gets AD in his or her diaper area. The skin stays too moist for AD.
What AD looks like in Children
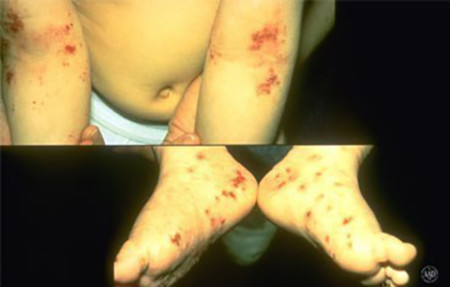
Common places
This 6-year-old boy has atopic dermatitis in the creases of his elbows and on his feet — common places for AD to appear in children.
When AD begins between 2 years of age and puberty, the child often has these signs and symptoms:
- A rash that often begins in the creases of the elbows or knees. Other common places for the rash to appear are the neck, wrists, ankles, and/or crease between the buttocks and legs
- Itchy, scaly patches where the rash appeared
In time, the skin with AD can:
- Get bumpy, looking like permanent goose bumps
- Lighten (or darken) where AD appears
- Thicken, turning leathery to protect itself from constant scratching
- Develop knots (only on the thickened skin)
- Itch all the time (only on the thickened skin)
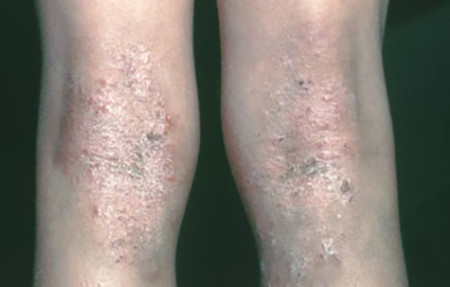
Thickened skin
This 7-year-old girl says the thickened skin on the back of her knees is always dry and always itches.
What it looks like in Adults
Patchy, scaly skin
Adults who have AD often have darker patches and scaly skin, as does this 30-year-old woman.

It is rare for adults to get AD. Most people (90%) get AD before age 5. About half (50%) of people who get AD during childhood continue to have milder signs and symptoms of AD as an adult. When an adult has AD, it often looks different from the AD of childhood. For adults, AD often:
- Appears in the creases of the elbows or knees and nape of neck
- Covers much of the body
- Can be especially noticeable on the neck and face
- Can be especially bad around the eyes
- Causes very dry skin
- Causes non-stop itch
- Causes scaly skin — more scaly than in infants and children
- Leads to skin infections
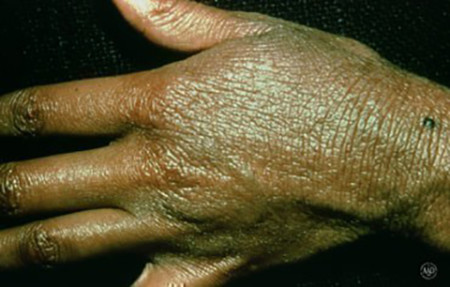
Itchy skin
Years of scratching caused permanently thickened skin on this woman’s hand and wrist. This skin always itches.
If a person has had AD for years, patches of skin may be thick and darker than the rest of the skin (or lighter). Thickened skin can itch all the time.
Adults who had AD as a child and no longer have AD can have the following:
- Extremely dry skin
- Skin that is easily irritated
- Hand eczema
- Eye problems (eczema on eyelids, cataracts)
How do dermatologists diagnose AD?
To diagnose atopic dermatitis (AD), a dermatologist begins by looking at the child’s skin. The dermatologist will look for a rash. The dermatologist also will ask questions. It is important for the dermatologist to know whether the child has itchy skin. The dermatologist also needs to know whether blood relatives have had AD, asthma, or hay fever.
Sometimes a dermatologist will perform a patch test. This medical test is used to find allergies. It involves placing tiny amounts of allergens (substances that cause allergies for some people) on the child’s skin. The dermatologist will check the skin for reactions. Checks are often done after a few hours, 24 hours, and 72 hours. Studies suggest that some allergens can make AD worse.
How do dermatologists treat AD?
Treatment cannot cure AD, but it can control AD. Treatment is important because it can:
- Prevent the AD from getting worse
- Calm the skin, relieving pain and itch
- Reduce emotional stress
- Prevent infections
- Stop the skin from thickening. Thickened skin often itches all the time — even when the AD is not flaring
A treatment plan often includes medicine, skin care, and lifestyle changes. Skin care and lifestyle changes can help prevent flare-ups. Many patients receive tips for coping. Doing all of this may seem bothersome, but sticking to the plan can make a big difference. A dermatologist will create a treatment plan tailored to the patient’s needs. Medicine and other therapies will be prescribed as needed to:
- Control itching
- Reduce skin inflammation (redness and swelling)
- Clear infection.
- Loosen and remove scaly lesions
- Reduce new lesions from forming
Outcome
Studies have found that when AD develops in an infant or young child, the child tends to get better with time. For some children, the condition completely disappears by age 2.
About half (50%) of the children who get AD will have it as an adult. The good news is that the AD often becomes milder with age.
There is no way to know whether the AD will go away or be a lifelong disease. This makes treatment very important. Treatment can stop the AD from getting worse. Treatment also helps to relieve the discomfort.
