Do you need an appointment?
Squamous Cell Carcinoma – The Second Most Common Skin Cancer
Squamous cell carcinoma (SCC) of the skin is the second most common form of skin cancer, characterized by abnormal, accelerated growth of squamous cells. When caught early, most SCCs are curable.
SCC of the skin is also known as cutaneous squamous cell carcinoma (cSCC). Adding the word “cutaneous” identifies it as a skin cancer and differentiates it from squamous cell cancers that can arise inside the body, in places like the mouth, throat or lungs.
What is a squamous cell?
One of three main types of cells in the top layer of the skin (the epidermis), squamous cells are flat cells located near the surface of the skin that shed continuously as new ones form.
SCC occurs when DNA damage from exposure to ultraviolet radiation or other damaging agents trigger abnormal changes in the squamous cells.
Risk Factors
Squamous cell carcinoma (SCC) of the skin is caused by DNA damage that leads to abnormal changes (mutations) in the squamous cells in the outermost layer of skin.
Understanding what causes this damage and the factors that increase your risk of developing SCC can help you detect the disease early or prevent it from happening in the first place.
These factors increase your SCC risk:
- Unprotected exposure to ultraviolet (UV) radiation from the sun or tanning beds.
- Weakened immune system due to illness or certain immunosuppressive medications.
- History of skin cancer, including basal cell carcinoma (BCC).
- Age over 50: Most SCCs appear in people over age 50.
- Fair skin: People with fair skin are at an increased risk for SCC.
- Gender: Men are more likely to develop SCC.
- Sun-sensitive conditions, including xeroderma pigmentosum.
- Chronic infections and skin inflammation from burns, scars and other conditions.
- Skin precancers, including actinic keratosis.
- History of human papilloma virus HPV
What does SCC look like?
SCCs can appear as scaly red patches, open sores, rough, thickened or wart-like skin, or raised growths with a central depression. At times, SCCs may crust over, itch or bleed. The lesions most commonly arise in sun-exposed areas of the body.
SCCs can also occur in other areas of the body, including the genitals.
Warning Signs
When caught promptly, almost all squamous cell carcinomas (SCCs) of the skin can be successfully treated. But when they become more advanced, these skin cancers can become dangerous.
That’s why it’s important to be on the lookout for any SCC warning signs, including new, changing or unusual skin growths.
How to spot a SCC
SCC of the skin can develop anywhere on the body but is most often found on exposed areas exposed to ultraviolet (UV) radiation like the face, lips, ears, scalp, shoulders, neck, back of the hands and forearms. SCCs can develop in scars, skin sores and other areas of skin injury. The skin around them typically shows signs of sun damage such as wrinkling, pigment changes and loss of elasticity.
SCCs can appear as thick, rough, scaly patches that may crust or bleed. They can also resemble warts, or open sores that don’t completely heal. Sometimes SCCs show up as growths that are raised at the edges with a lower area in the center that may bleed or itch.
SCCs can also look different from the descriptions above. If you notice anything unusual, such as a sore that fails to heal, or a new spot, make an appointment with our office.
The following pictures show many of the ways that SCC can appear on the skin.
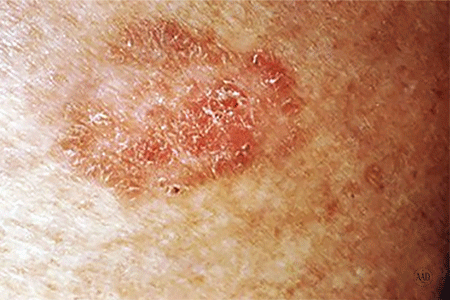
Rough-feeling, reddish patch
This is an early sign of squamous cell carcinoma.
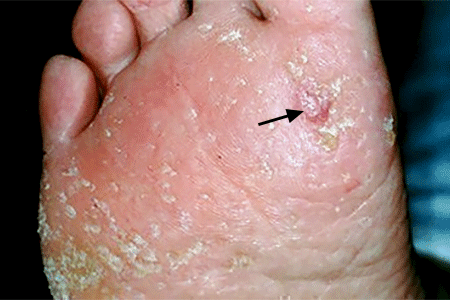
Round growth with raised borders
This squamous cell carcinoma developed from a pre-cancerous growth called an actinic keratosis.
A sore that won’t heal or heals and returns
On the skin or lips, squamous cell carcinoma can look like a sore.
Age spot
This can be a sign of squamous cell carcinoma, which is why you want a board-certified dermatologist to examine your skin before you treat any age spot.
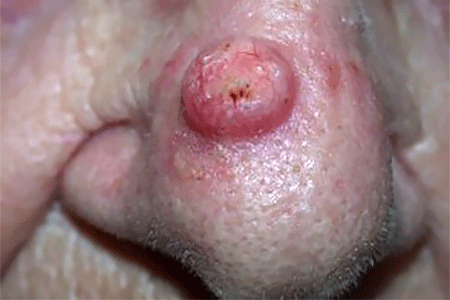
Raised, round growth
This is a common sign of squamous cell carcinoma of the skin.
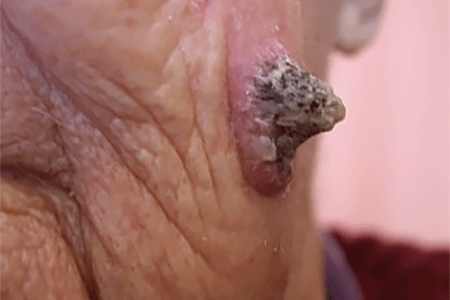
Animal’s horn
When squamous cell carcinoma looks like this, it tends to grow quickly.
What you can do
Examine yourself head to toe once a month: Keep an eye out for new or changing lesions that grow, bleed, or do not heal. Learn how to check your skin here.
When in doubt, check it out. Follow your instincts and visit your doctor if you see a spot that just doesn’t seem right.
See your dermatologist for a professional skin exam every year even if you don’t see anything suspicious. These specialists are skilled at identifying and treating abnormal skin growths that may be undetectable to the untrained eye and can check areas of your body that are difficult for you to see yourself.
Follow up regularly: Especially if you’ve already had either SCC or basal cell carcinoma (BCC), melanoma or precancers like actinic keratosis, be sure to see your dermatologist for a skin exam at recommended intervals.
Practice sun safety: Making daily sun protection a part of your lifestyle is the single most effective way to reduce your risk of developing skin cancer.
How dangerous is SCC?
While the majority of SCCs can be easily and successfully treated, if allowed to grow, these lesions can become disfiguring, dangerous and even deadly. Untreated SCCs can become invasive, grow into deeper layers of skin and spread to other parts of the body.
Treatment
Most squamous cell carcinomas (SCCs) of the skin can be cured when found and treated early. Treatment should happen as soon as possible after diagnosis, since more advanced SCCs of the skin are more difficult to treat and can become dangerous, spreading to local lymph nodes, distant tissues and organs.
If you’ve been diagnosed with an SCC that has not spread, there are several effective treatments that can usually be performed on an outpatient basis. The choices available to you depend on the tumor type, size, location and depth, as well as your age and overall health.
Options include:
- Excisional surgery
- Mohs surgery
- Cryosurgery
- Radiation
- Photodynamic therapy (PDT)
- Topical medications
Ask your dermatologist to clearly explain the options that might work best for you, including details about the risks and benefits. Visit our skin cancer treatment page for more details on each.