Schedule a dermatology appointment?
Psoriasis
As one of the most common chronic skin conditions, psoriasis (suh-rye-ah-sis) is known for causing silver, scaly patches of plaque on your skin, as well as inflammation and discomfort.
Psoriasis is a condition that causes the body to make new skin cells in days rather than weeks. As these cells pile up on the surface of the skin, you may see thick, scaly patches.
Plaque psoriasis is the most common type of psoriasis
Those thick, scaly patches that develop on the skin are called plaques (placks). About 80% to 90% of people living with psoriasis get plaques, so they have plaque (plack) psoriasis.
Plaques can appear anywhere on the skin, but you’re most likely to find them on the:
- Knees
- Elbows
- Lower back
- Scalp
Plaques tend to vary in size. They may appear on the skin as a single patch or join together to cover a large area of skin. No matter the size, plaques tend to be itchy. Without treatment, the itch can become intense. Some people notice that their skin stings, burns, or feels painful and tight.
Psoriasis is often a life-long disease
Most people who get psoriasis have it for life. That’s true no matter what type of psoriasis you have, with one exception. Some children who have guttate (gut-tate) psoriasis see their psoriasis go away. Because psoriasis tends to be a life-long disease, it helps to learn about it and see a board-certified dermatologist. A bit of knowledge and help from a board-certified dermatologist can give you some control over the psoriasis. By gaining control, you can see clearer (or clear) skin. Gaining control can also help you to feel better, improve your overall health, and prevent the psoriasis from worsening.
Gaining control often involves:
- Learning (and avoiding) what triggers your psoriasis
- Sticking to a good psoriasis skin care routine
- Living a healthy lifestyle
- Using medication when necessary
Seeing a board-certified dermatologist has another benefit. Psoriasis can increase your risk of developing certain diseases, such as psoriatic arthritis or diabetes. Your dermatologist can watch for early signs of disease. If you do develop another disease, early treatment helps to prevent the disease from worsening. When you see a board-certified dermatologist about psoriasis, your dermatologist may talk about the type(s) of psoriasis you have. It’s possible to have more than one type.
Psoriasis Q & A
What causes psoriasis?
Your skin sheds dead cells and regenerates new cells on a daily basis. This continuous cycle is essential for having healthy skin. When you 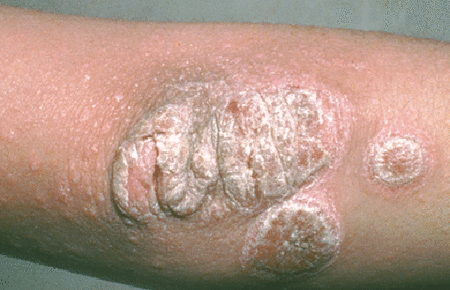
Even though the exact cause isn’t known, dermatologists find that you’re more likely to suffer from this chronic condition if you have a family history. It’s believed that psoriasis leads to faulty signals in your body’s immune system, which results in the overproduction and accelerated growth of skin cells. Common triggers of flare-ups include:
- Bacterial or viral infections
- Skin injuries
- Stress or anxiety
- Vitamin D deficiency
- Skin injury, including tattoos and piercings
- Shaving
- Smoking or exposure to secondhand smoke
- Drinking frequently or drinking in excess
- Certain medications that are used to treat high blood pressure or bipolar disorder
- Dry, cold weather
- Sunburns
- Spending time in air conditioned areas
Symptoms
With psoriasis, you may experience:
- Red patches covered in silvery scales
- Thickened patches of skin
- Itching or burning skin
- Thickened or ridged nails
It’s also common for sufferers to have stiff and swollen joints, which can mimic the symptoms of arthritis.
Treatment
Treating psoriasis involves working to reduce inflammation, clear your skin, and prevent future flare-ups. While psoriasis can’t be cured, 
You’ll find many products to treat psoriasis that you can buy without a prescription. Your dermatologist may refer to these products as “over-the-counter” (OTC) treatments. No matter what you call them, these products work best for people who have very mild psoriasis, with one exception. Moisturizers can benefit anyone who has psoriasis.
Dermatologists recommend applying moisturizer once a day, and more often when your skin is really dry. When shopping for a moisturizer, you want to select a:
- Heavy cream, ointment, or oil rather than a lotion
- Fragrance-free product
- Product that you like and will use
Oil can be especially healing, but it’s also messy. To reap the benefits of oil, try applying it before bedtime.
Dermatologists can tailor psoriasis treatment to the type of psoriasis you have. Sometimes, this requires combining treatments. You may also need one treatment plan to gain control over your psoriasis and another to maintain the results. There are many options for a comprehensive treatment plan, which can include:
- Scale softeners – a warm, not hot, bath prior to applying scale softeners helps them work better
- Scale softeners can allow other treatments and moisturizers work more effectively by removing the scale.
- Products containing coal tar
- An anti-itch product
- Topical corticosteroids
- Vitamin D creams
- Medications to slow skin cell growth
- Topical or oral retinoids (vitamin A)
We can also help you find clinical-grade moisturizers and cosmetics that are designed for sensitive skin. While these solutions won’t heal psoriasis, they can certainly reduce dryness and itching, and even prevent future flare-ups.
Some psoriasis sufferers find relief by going through phototherapy, which involves exposing your skin to controlled amounts of light. These treatments often minimize redness and stimulate skin healing.
Biologics
Biologics are newer, stronger medicines. A biologic can target, or quiet, only the part of the immune system that is overactive because of psoriasis. This means that biologics have less risk of causing problems with the liver, kidneys, and other organs than do other strong psoriasis medicines.
A biologic is an important treatment option for people with moderate-to-severe psoriasis, psoriatic arthritis, or both. For many people, taking a biologic was life changing because it helped control their symptoms when other treatments failed.
Safety: Overall, the biologics have a good safety record.
A patient’s risk of developing a serious infection remains the biggest concern. For this reason, dermatologists carefully screen each patient before prescribing a biologic.
You’ll need to have some medical tests before your dermatologist can tell whether a biologic can be prescribed to treat your psoriasis. Blood tests and tuberculosis (TB) testing are typically required. Some patients need additional medical tests.
Effectiveness: Studies show that the biologics approved to treat psoriasis and psoriatic arthritis can be very effective. For many people with moderate-to-severe psoriasis or psoriatic arthritis, a biologic may offer the most effective treatment available.
If you take a biologic continuously, it tends to be more effective. Stopping and starting can cause a biologic to lose its effectiveness and may cause certain side effects.
It’s also possible for a biologic to stop working after a person takes it for some time. If this happens, another biologic may work.
While a biologic can lose its effectiveness over time, studies show that for many people a biologic remains an effective and safe treatment for years.
There are some more great resources on ways to ease the symptoms on the American Academy of Dermatology’s website.
We recommend booking a psoriasis evaluation by requesting an appointment online, or by calling our offices.
